In most mature networks, especially those with higher volumes and greater velocity, population demand tends to persist. Sharp, sudden deviations are unusual and almost always result from externalities. Even in these atypical circumstances, it is often not so much that demand itself has changed as the ability to express continued demand has somehow been displaced.
There are exceptions, but when in doubt, placing my bets on the persistence of well-established pull usually pays off.
Consistent with this Supply Chain Resilience principle, last summer I joined many others to suggest that preexisting patterns of demand for seasonal flu vaccinations would help target where extra effort would be needed to encourage covid vaccinations. Not much was done last summer — many who might have done more were plenty busy with the sick and dying. I pushed again last November. Once again, there were — I agree — competing priorities. Others more credible than me continued pushing. But serious grass-roots engagement with vaccine reluctance has been rare until recently.
Still, the data are fairly clear: places with persistently low demand for seasonal flu vaccinations are also places with lower covid vaccination rates. In 2019-2020, 51.8 percent of US residents were vaccinated for seasonal flu (a bit better than in most flu seasons). As of July 18, 2021, the United States had fully vaccinated 48.6 percent of its population against covid. The chart below shows those states with the lowest seasonal flu vaccination rates for 2019-2020. The third column reports the population percentage in each of these states fully vaccinated for covid.
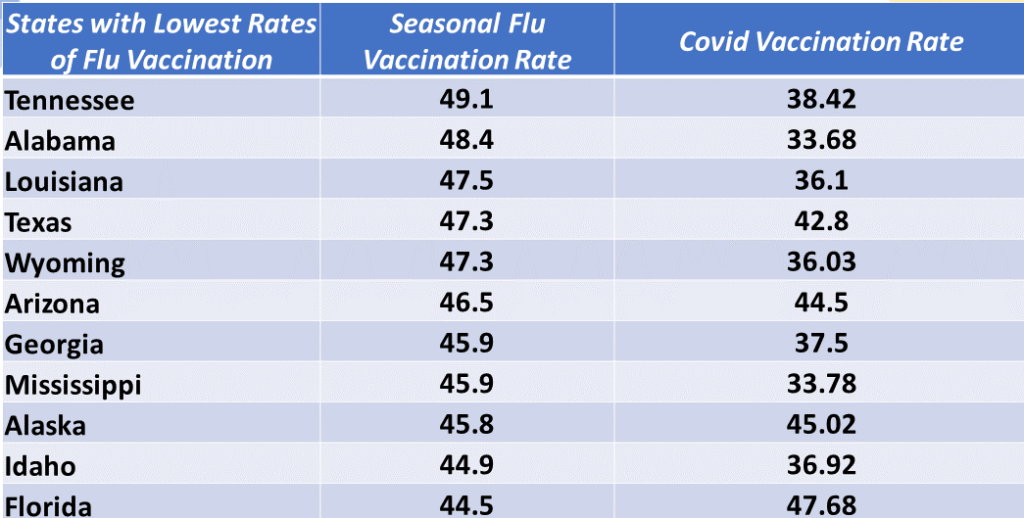
There are outliers. Arkansas vaccinated 54.9 percent of it’s population against seasonal flu, but so far only 35.39 percent are vaccinated against covid. Florida’s three point improvement in covid coverage versus the seasonal flu is better than many states (but not as good as Vermont moving from 57 percent for flu to 66.9 percent for covid). I wish I had time to run a Pearson’s R on the correlation between flu and covid vaccinations rates. (I’m sure someone has this, please let me know.)
It would also be interesting to know more about what happened in Arkansas and Vermont that might explain how prior patterns were undone. But the larger pattern is still clear enough.
Current resistance to vaccinations should not be surprising. Given long-established patterns with seasonal flu vaccinations, we should not assume recent causes. We should also avoid being distracted by ad-hoc (even post-hoc) justifications that will obscure deeper sources of resistance (potentially obscure even to the resistant, reluctant, hesitant, and delayed). Especially after losing so much time and opportunity, there is even greater urgency to understand and engage real impediments. It is also worth being realistic regarding the time-and-effort typically involved with demand creation.
The coronavirus called “novel” in late 2019 was not optimized for human infection. The Delta (B.1.617.2) variant of that original virus is much more effective at claiming human hosts. Fortunately, so far, vaccines approved in the US have demonstrated considerable ability to suppress the onset of disease, even by Delta. Unfortunately, the virus will continue to evolve. Over half of the US population and nearly three-quarters of the world population are, right now, essentially high capacity — unvaccinated — mutation factories.
The more who are effectively vaccinated sooner, the less likely a vaccine-vanquishing mutation.
+++
July 27 UPDATE: Many thanks to a reader who sent along this link to a related BBC report.